Vaccines are one of the most effective public health tools ever developed. They have helped prevent outbreaks, reduced severe illness, and saved millions of lives across generations. Despite this, misinformation about vaccines continues to circulate widely, especially online. False claims can sound convincing when repeated often enough, even when they are not supported by science. This creates confusion, fear, and hesitation that can put individuals and entire communities at risk.
Understanding how vaccines work and why they are recommended is essential in an age where information spreads quickly but accuracy does not always keep pace. Many vaccine myths are rooted in outdated studies, misinterpreted data, or emotional anecdotes that lack scientific evidence. Others arise from mistrust in institutions or a misunderstanding of how the immune system responds to vaccines. Addressing these concerns requires patience, clarity, and a focus on credible research rather than speculation.
Vaccines undergo extensive testing before they are approved for public use, and their safety continues to be monitored long after they are introduced. Scientists, doctors, and public health experts around the world rely on decades of data to make recommendations designed to protect both individuals and communities. When vaccination rates are high, diseases struggle to spread. When rates drop, outbreaks can and do return.
We take a closer look at ten of the most common vaccine myths and contrasts them with well established scientific facts. The goal is not to shame or dismiss questions, but to provide clear and reliable information that helps readers make informed decisions. By separating truth from misinformation, we can better understand why vaccines remain a cornerstone of modern medicine and why accurate knowledge matters for personal health and public safety.
Image
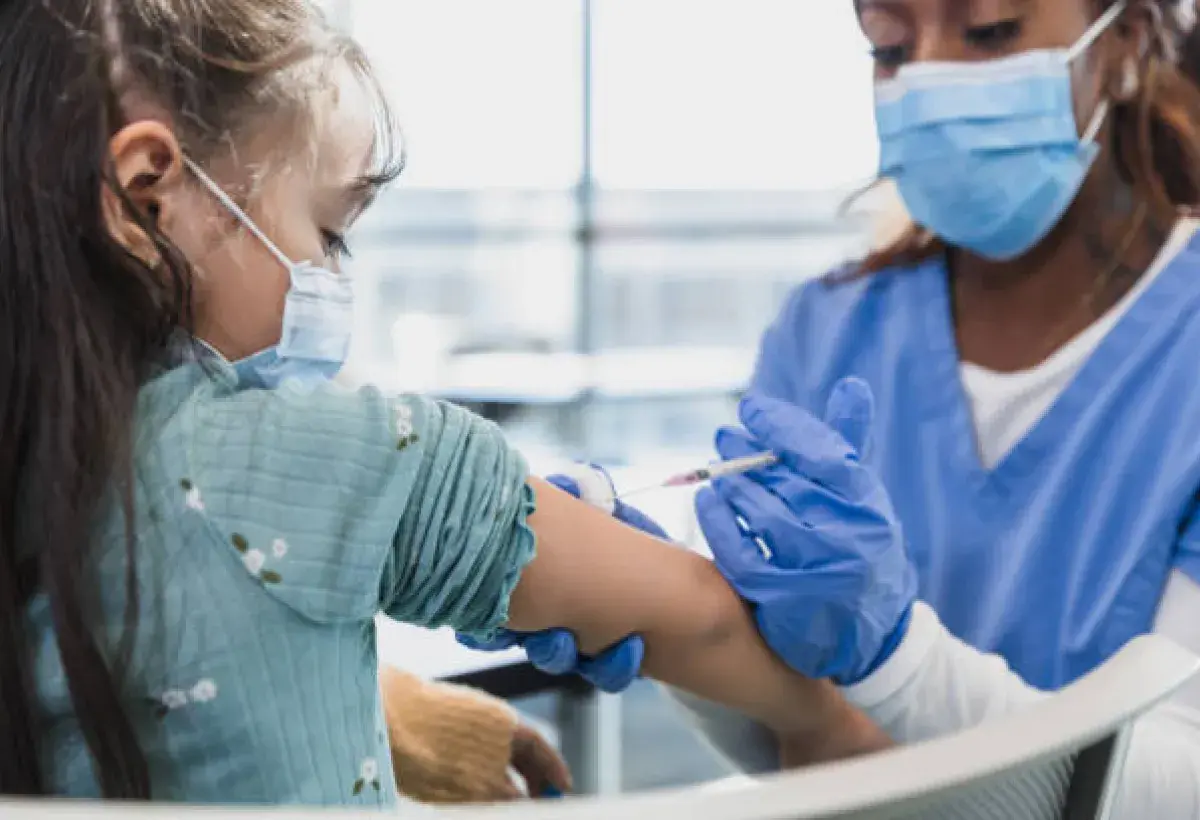
Myth 1: Vaccines cause autism
The belief that vaccines cause autism is one of the most persistent myths in modern medicine, despite being thoroughly disproven. This idea originated from a small study published in the late nineteen nineties that claimed a link between a childhood vaccine and autism. That study was later found to contain serious ethical violations and flawed data, leading to its full retraction. The author also lost his medical license, yet the claim continued to spread.
Since then, researchers around the world have conducted large scale studies involving hundreds of thousands of children. These studies compared vaccinated and unvaccinated populations and consistently found no difference in autism rates. The evidence clearly shows that vaccines do not cause autism. Autism is now understood to be a neurodevelopmental condition influenced by genetics and early brain development, not by immunizations.
One reason this myth persists is timing. Signs of autism often become noticeable around the same age when children receive certain vaccines. This coincidence can create the false impression of cause and effect. However, correlation does not mean causation, and scientific studies are designed specifically to test whether such links truly exist. In this case, they do not.
Continuing to repeat this myth can have serious consequences. Fear of autism has led some parents to delay or skip vaccinations, increasing the risk of preventable diseases. Measles outbreaks in recent years are one example of what happens when vaccination rates decline. Protecting children means relying on evidence based medicine rather than discredited claims.
Image

Myth 2: Natural immunity is better than vaccine induced immunity
Natural immunity occurs after a person becomes infected with a disease and recovers, while vaccine induced immunity develops without the person having to suffer the illness itself. Some people believe natural immunity is stronger or healthier, but this belief ignores the risks involved in getting sick in the first place. Many infectious diseases can cause severe complications, long term damage, or death, even in otherwise healthy individuals.
Vaccines are designed to train the immune system in a controlled and safe way. They expose the body to a harmless part of a virus or bacterium or an inactivated form that cannot cause disease. This allows the immune system to learn how to recognize and fight the real pathogen later. In many cases, the immunity produced by vaccines is just as strong as natural immunity, and sometimes even more reliable.
Relying on natural infection means accepting the possibility of hospitalization, chronic health problems, or spreading the disease to others. For example, chickenpox can lead to pneumonia or brain inflammation, and measles can suppress the immune system long after recovery. Vaccines prevent these risks while still providing protection.
Public health strategies prioritize vaccines because they reduce suffering on a large scale. Choosing vaccination is not about avoiding immunity but about gaining protection without unnecessary danger. Scientific evidence consistently shows that vaccine induced immunity offers a safer path to disease prevention for individuals and communities alike.
Image
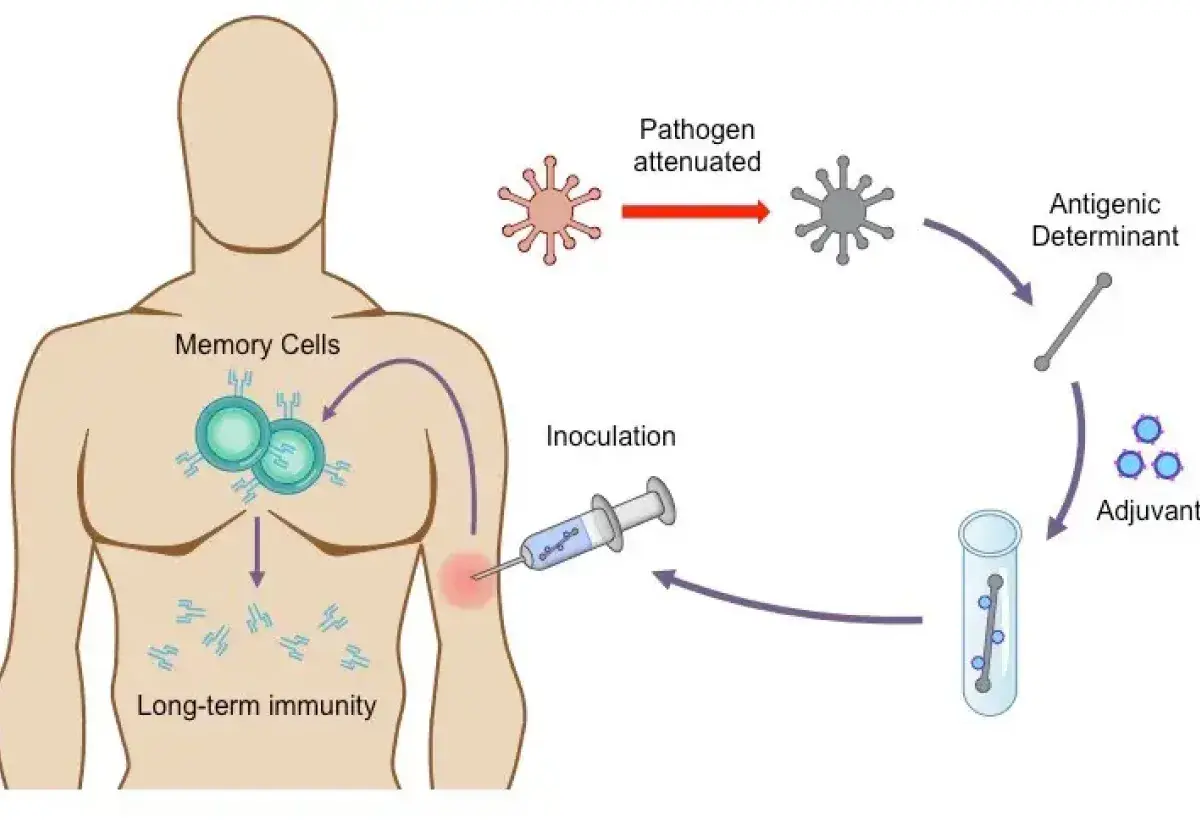
Myth 3: Vaccines contain harmful toxins
Concerns about vaccine ingredients are common, especially when people encounter unfamiliar chemical names. Some vaccines contain substances like aluminum salts or trace amounts of formaldehyde, which can sound alarming without proper context. In reality, these ingredients are used in extremely small amounts and serve specific purposes, such as improving the immune response or ensuring vaccine stability.
Aluminum is one of the most abundant elements in the environment. Humans are exposed to it daily through food, water, and even breast milk. The amount of aluminum in vaccines is far lower than what people naturally consume over time. Formaldehyde is also produced naturally by the human body as part of normal metabolic processes. The trace amounts used in vaccines are well within established safety limits.
Before approval, vaccine ingredients are carefully evaluated for safety by regulatory agencies. These evaluations consider cumulative exposure, vulnerable populations, and long term effects. If an ingredient posed a real danger at the levels used, it would not be included.
Misinformation often focuses on ingredient names without explaining dosage or biological context. Toxicity depends on amount, not just presence. Water and oxygen are essential for life, yet harmful in extreme quantities. Vaccines use ingredients in precise doses that have been proven safe and effective through rigorous testing.
Image
Myth 4: Too many vaccines overload the immune system
Some parents worry that receiving multiple vaccines, especially in early childhood, might overwhelm a child’s immune system. This concern is understandable, but it does not align with how the immune system actually works. From the moment a baby is born, their immune system encounters thousands of bacteria and viruses every day through normal activities like eating and breathing.
Modern vaccines contain fewer antigens than vaccines from decades ago, even though they protect against more diseases. An antigen is the part of a germ that triggers an immune response. The total number of antigens in the recommended vaccine schedule is only a tiny fraction of what the immune system handles naturally on a daily basis.
Scientific studies have shown that children who receive multiple vaccines at once do not have higher rates of infections or immune related problems. In fact, spreading out vaccines can leave children vulnerable for longer periods, increasing the risk of serious illness.
The recommended vaccine schedule is designed based on extensive research to provide protection at the most effective times. It balances safety, immune response, and disease risk. Rather than overwhelming the immune system, vaccines help prepare it to respond quickly and effectively when real threats appear.
Image

Myth 5: Only kids need vaccines
Vaccination is often associated with childhood, but protection does not stop after adolescence. Adults also need vaccines to maintain immunity and protect against diseases that can become more dangerous with age. Some childhood vaccines require boosters because immunity can decrease over time.
Seasonal influenza vaccines are recommended annually for adults because flu viruses change frequently. Older adults are also advised to receive vaccines against shingles and pneumonia, which can cause severe complications later in life. Pregnant individuals may need certain vaccines to protect both themselves and their babies.
Adults can also be a source of infection for vulnerable populations, including infants and people with weakened immune systems. Staying up to date on vaccinations helps reduce the spread of disease in workplaces, households, and communities.
Vaccination is a lifelong health practice, not a one time childhood event. By continuing to follow vaccine recommendations throughout adulthood, individuals contribute to their own well being and help protect those around them.
Image
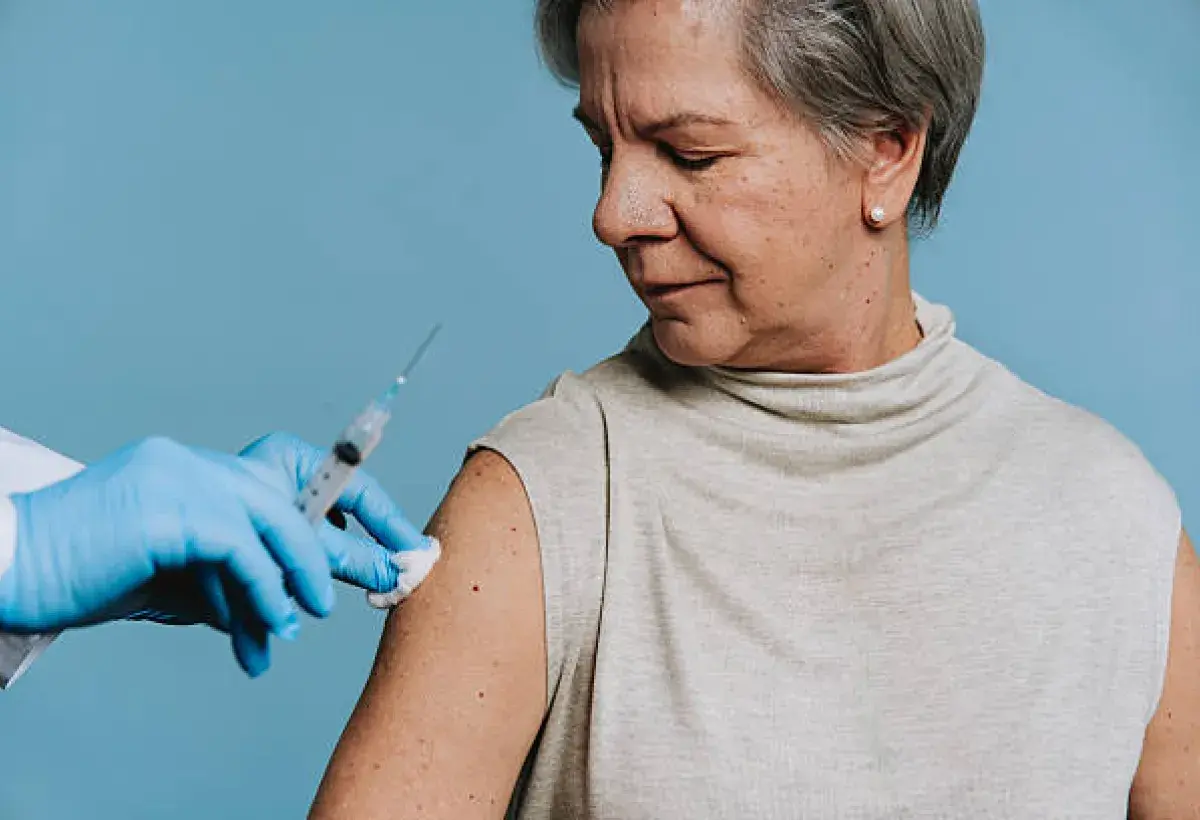
Myth 6: If others are vaccinated, I do not need to be
This myth misunderstands how community protection works. When a large portion of a population is vaccinated, diseases have fewer opportunities to spread. This effect, often called herd immunity, helps protect people who cannot be vaccinated due to medical conditions. However, it only works when vaccination rates remain high.
If too many individuals choose not to vaccinate, community protection weakens. This can lead to outbreaks, even of diseases that were once considered under control. Measles outbreaks in recent years have often occurred in areas with lower vaccination coverage.
Choosing not to vaccinate while relying on others creates an unfair burden on the community. It increases risk for infants, elderly individuals, and those with compromised immune systems. Vaccination is not just a personal decision but a shared responsibility.
By getting vaccinated, individuals help maintain the protective barrier that keeps dangerous diseases from spreading widely. Community health depends on collective participation, not assumptions that others will carry the responsibility alone.
Image

Myth 7: Vaccines are not tested enough
Vaccines are among the most thoroughly tested medical products available. Before approval, they go through multiple phases of clinical trials involving thousands of participants. These trials evaluate safety, effectiveness, dosage, and potential side effects. Only after meeting strict standards are vaccines approved for public use.
Testing does not stop after approval. Ongoing monitoring systems track vaccine safety in real world conditions. Health agencies continuously review data and investigate any reported adverse events. This allows rare side effects to be identified quickly and addressed.
The idea that vaccines are rushed or inadequately tested often overlooks this extensive process. While development timelines can vary, safety requirements remain consistent. Advances in technology and global collaboration can speed up research without skipping critical steps.
Trust in vaccines is built on transparency and evidence. Decades of data support their safety and effectiveness. Claims that vaccines are insufficiently tested are not supported by the rigorous systems in place worldwide.
Image

Myth 8: Vaccines can cause the disease they are meant to prevent
Most vaccines cannot cause the disease they protect against. Many use inactivated viruses, weakened components, or specific proteins that are incapable of causing illness. These elements are enough to stimulate an immune response without triggering full infection.
In rare cases, people may experience mild symptoms after vaccination, such as a low fever or soreness. These reactions are signs that the immune system is responding, not that the disease has developed. They are typically short lived and far less severe than the actual illness.
Live attenuated vaccines use a weakened form of a virus, but even these are designed to be safe for the vast majority of people. Serious complications are extremely rare and carefully monitored.
Confusing side effects with disease contributes to unnecessary fear. Understanding how vaccines are formulated helps clarify why they protect rather than harm. The risk of illness from vaccination is dramatically lower than the risk posed by natural infection.
Image
Myth 9: Better hygiene alone wiped out diseases, not vaccines
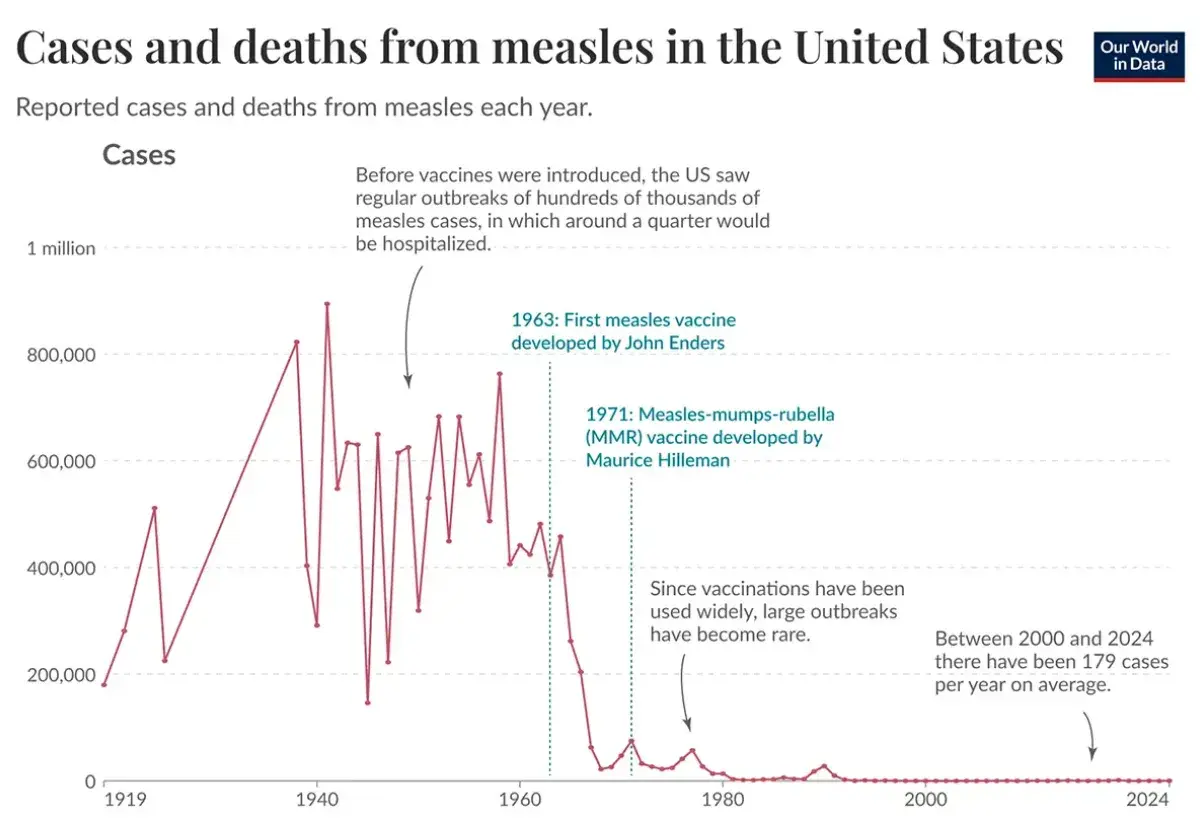
Improved sanitation, clean water, and better hygiene have played important roles in reducing disease, but they do not fully explain the dramatic decline of many infectious illnesses. Historical data shows that diseases like measles and polio continued to cause widespread illness even after hygiene improved. Significant drops occurred only after vaccines were introduced.
Hygiene helps prevent the spread of some infections, but it cannot stop viruses that are highly contagious through the air. Measles, for example, can linger in the air long after an infected person leaves a room. Vaccination is the most effective way to prevent such diseases.
Countries that introduced vaccination programs saw rapid declines in cases. When vaccination rates fell, these diseases often returned, despite continued improvements in hygiene. This pattern highlights the critical role vaccines play.
Public health success is the result of multiple strategies working together. Hygiene and vaccination complement each other, but vaccines remain essential for controlling many serious diseases.
Image
Myth 10: Vaccines are only about personal choice
Vaccination decisions affect more than just the individual. Infectious diseases spread through communities, and one person’s choice can impact many others. People who cannot be vaccinated, such as newborns or those undergoing certain medical treatments, rely on others for protection.
High vaccination rates reduce the chance of outbreaks and protect healthcare systems from being overwhelmed. When preventable diseases spread, resources are diverted from other medical needs, affecting overall care quality.
Framing vaccination purely as personal choice ignores the shared nature of public health. Just as traffic laws exist to keep everyone safe, vaccination recommendations aim to protect the population as a whole.
Choosing vaccination is both a personal health decision and a contribution to community safety. Recognizing this shared responsibility helps build healthier and more resilient societies.
Image

Vaccine misinformation thrives in environments where fear outweighs facts and where complex science is reduced to misleading sound bites. Addressing these myths requires more than simply stating that they are wrong. It requires explaining why they are wrong and presenting evidence in a clear and accessible way. When people understand how vaccines work, why they are tested, and how they protect both individuals and communities, fear often gives way to confidence.
The myths discussed in this article share a common theme of misunderstanding. Whether it is confusion about ingredients, immune system capacity, or personal choice, these claims overlook decades of scientific research and real world experience. Vaccines have repeatedly proven their value by preventing suffering, disability, and death on a massive scale.
Making informed health decisions means relying on credible sources and being willing to question information that lacks evidence. It also means recognizing the role each person plays in protecting those around them. Vaccination is not just about avoiding illness today, but about ensuring a safer future for everyone.
By separating truth from misinformation, we can move toward conversations grounded in knowledge rather than fear. Vaccines remain one of the strongest tools we have to protect public health, and understanding the facts behind them is an important step toward building trust, resilience, and healthier communities.
Image

References
• World Health Organization GACVS vaccine safety statement on autism. World Health Organization
• PAHO debunking immunization myths. Pan American Health Organization
• CDC vaccine safety page on autism and research reviews. CDC Beta
• AAAAI vaccine myths and facts guide. AAAAI
• publichealth.org vaccine safety guide on ingredients. publichealth.org
• UNICEF immunization myths and facts. UNICEF
• Philadelphia Immunization Program vaccine facts. vaccines.phila.gov
• PatientGuide vaccine myths and effectiveness overview. patientguide.io









